Understanding the Cornea and Its Role in Vision
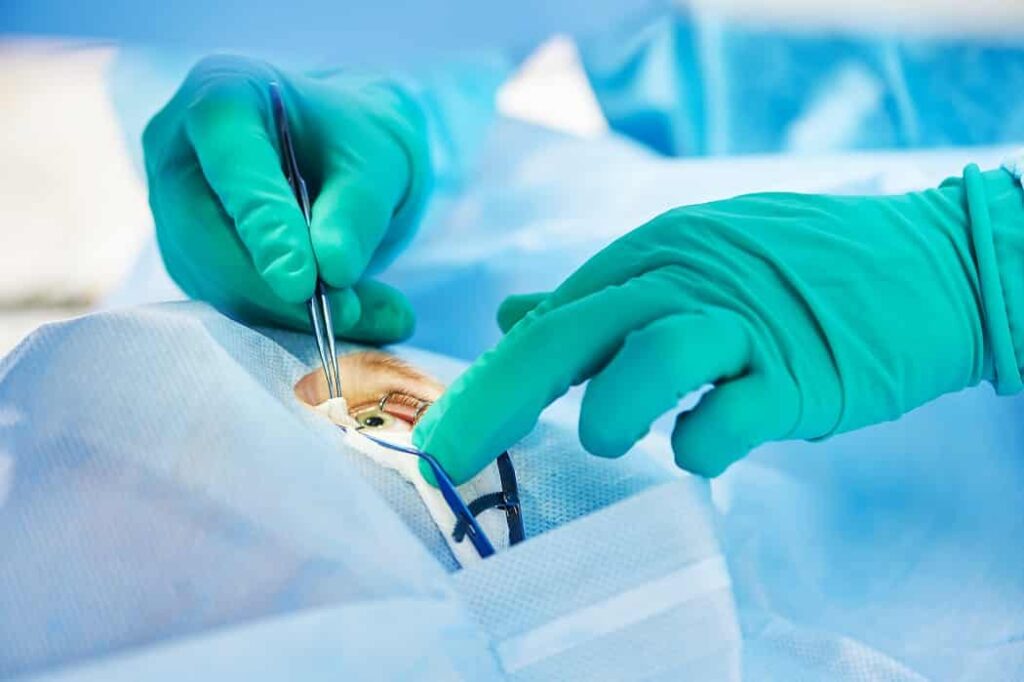
The cornea is the eye’s transparent outer layer that acts like a window, letting light enter and focusing it onto the retina. A healthy cornea is essential for sharp vision, and even minor damage can cause blurred or distorted sight. It consists of several layers: the epithelium, stroma, and endothelium, each serving a unique function. The epithelium shields the eye from debris and germs, while the stroma provides structural support. The endothelium maintains fluid balance, ensuring clarity. Conditions like infections, injuries, or degenerative diseases can compromise these layers, reducing vision quality. Understanding the cornea’s structure highlights why corneal transplants are sometimes the only solution to restore sight.
What Happens During a Corneal Transplant
A corneal transplant, also called keratoplasty, replaces a damaged cornea with healthy donor tissue. The procedure varies based on the damage, ranging from full-thickness transplants to partial-layer replacements. The main types are:
- Penetrating keratoplasty – replacing all corneal layers
- Lamellar keratoplasty – replacing only affected layers
- Endothelial keratoplasty – targeting the innermost layer while preserving others
Surgeons carefully match donor tissue to the patient’s eye to reduce the risk of rejection. The operation usually takes one to two hours and is performed under local or general anesthesia. After surgery, the new cornea is secured in place, and immediate care is essential for a successful recovery.
Conditions That Require a Corneal Transplant
Corneal transplants are performed when the cornea cannot function properly due to damage or disease. Common reasons include:
- Corneal scarring from infections or injuries
- Keratoconus, a condition causing the cornea to thin and bulge
- Corneal dystrophies, which are inherited disorders
- Complications from prior eye surgeries
- Chemical or traumatic eye injuries
These conditions can severely affect vision, making a transplant the most effective way to restore clarity. Proper assessment by an ophthalmologist ensures the procedure is tailored to the patient’s specific needs.
Preparing for a Corneal Transplant
Before surgery, patients undergo a series of evaluations to assess eye health. Tests measure corneal thickness, shape, and overall condition. The type of transplant is determined by the extent of damage and patient factors. Selecting the right donor cornea is critical; surgeons look for healthy tissue free from disease. Patients are advised on what to expect during recovery, including activity restrictions and medications. Emotional preparedness is equally important, as the recovery process requires patience. Open communication with the eye care team ensures realistic expectations and peace of mind.
Step-by-Step Procedure
During surgery, anesthesia ensures comfort and prevents pain. The damaged corneal tissue is carefully removed, and the donor cornea is precisely placed in its position. Sutures may be used to secure the tissue, with some advanced techniques using finer or dissolvable stitches. High-precision microscopes and surgical tools allow surgeons to operate with accuracy. The operation usually lasts between one and two hours. After surgery, the eye is monitored closely for intraocular pressure and proper alignment of the new cornea. Patients are usually given protective eyewear and instructed on immediate post-surgery care.
Recovery Process
Healing from a corneal transplant can take several weeks to months. Patients may experience blurred vision, mild discomfort, or swelling initially. Eye drops containing antibiotics and anti-inflammatory medications are prescribed to prevent infection and reduce inflammation. Regular follow-up visits allow doctors to monitor healing progress and detect potential complications. Strenuous activities should be avoided, and protective measures like sunglasses are recommended. Patience is key, as the vision may continue improving gradually over time. Following all postoperative instructions increases the chances of a successful outcome.
Risks and Complications
While corneal transplants are generally safe, certain risks exist. Graft rejection is a primary concern, with symptoms including redness, light sensitivity, blurred vision, and discomfort. Other complications may include infection, suture problems, and increased intraocular pressure. Long-term risks can include recurrence of the original corneal condition or gradual thinning of the transplanted tissue. Preventive care, such as consistent use of prescribed eye drops and regular eye exams, reduces these risks. Prompt recognition and treatment of complications significantly improve outcomes. Being informed about potential risks helps patients take proactive measures during recovery.
Expected Outcomes
Most patients experience noticeable improvement in vision within a few weeks after the surgery, though full recovery can take up to a year. Success depends on factors like the patient’s age, overall eye health, and adherence to follow-up care. Some individuals may need glasses or contacts to optimize vision after the transplant. Routine assessments allow doctors to ensure the cornea remains clear and healthy. Recovery not only restores vision but also enhances daily life and independence. Patients who follow care instructions and maintain eye protection usually see the best results. Understanding the healing process helps manage expectations and build confidence in the procedure.
Advancements in Corneal Transplantation
Medical technology continues to improve outcomes for corneal transplant patients. Endothelial keratoplasty allows selective replacement of damaged corneal layers, leading to faster recovery and reduced risk. Research in stem cell therapy is providing new ways to repair corneal tissue without full transplantation. Artificial and bioengineered corneas offer solutions for patients without suitable donor tissue. Advanced imaging and surgical instruments allow for more precise and safer procedures. Immunomodulation research aims to prevent graft rejection and prolong corneal health. These innovations provide patients with better options, reduced risks, and improved quality of life.
Living With a Transplanted Cornea
Post-transplant life requires ongoing attention and lifestyle adjustments. Patients should protect their eyes from injury, avoid direct UV exposure, and use prescribed medications as directed. Routine eye exams ensure early detection of any complications. Activities like swimming or contact sports may require temporary modifications. Long-term success depends on consistency in follow-up care and healthy habits. Many patients regain independence in daily activities and enjoy significantly improved vision. Emotional and social support can also enhance adjustment to life after surgery.
Frequently Asked Questions (FAQ)
How long does a corneal transplant last?
Corneal transplants can last from 10 to 20 years or more, depending on individual health and type of procedure.
Can a corneal transplant be rejected?
Yes. Symptoms like redness, blurred vision, light sensitivity, or pain should prompt immediate medical attention. Early treatment often prevents permanent damage.
Will I need glasses after surgery?
Some patients require glasses or contact lenses for optimal vision, depending on preexisting conditions and post-surgery healing.
Is the surgery painful?
Anesthesia prevents pain during the procedure. Mild soreness or irritation may occur during recovery and is manageable with medication.
When can I resume normal activities?
Light daily activities can resume within weeks, but strenuous activity or swimming is generally restricted for several months.
Can both eyes be operated on at the same time?
Typically, transplants are staged to allow the first eye to heal before the second undergoes surgery. This reduces risks and allows for better monitoring.
Takeaway
Corneal transplant surgery provides hope and renewed vision for patients with damaged or diseased corneas. Careful preparation, expert surgical techniques, and diligent follow-up are essential for a successful outcome. Advances in medical technology and tissue engineering continue to enhance safety and effectiveness. Recovery requires patience, protective measures, and consistent adherence to postoperative care. With proper guidance and support, patients can enjoy restored vision, improved daily life, and renewed independence. Understanding the procedure and its possibilities empowers individuals to take control of their eye health and embrace the benefits of modern ophthalmology.